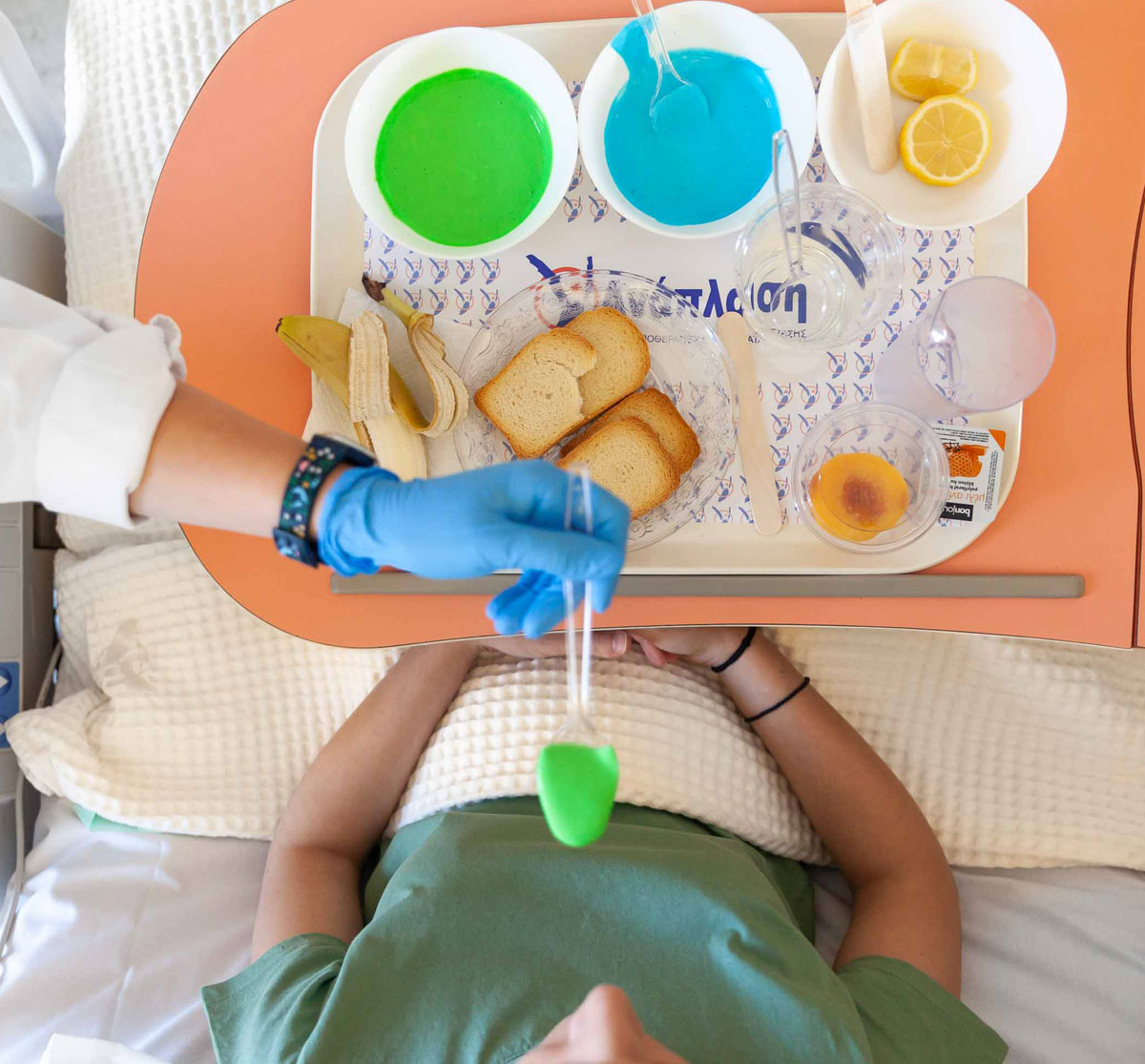
Στην ΑΝΑΠΛΑΣΗ ο ειδικός θεραπευτής, ως μέλος της Υπερ-Τομεακής Ομάδας Αποκατάστασης είναι εκπαιδευμένος στη χρήση διεθνώς αναγνωρισμένων θεραπευτικών τεχνικών (halliwick, bad ragaz, watsu) και εφαρμόζει εξατομικευμένο πρόγραμμα στον ασθενή.
Γιατί Εμάς

Σύγχρονες Εγκαταστάσεις Αποκατάστασης

Εξειδικευμένο & Έμπειρο Προσωπικό

Τεχνολογία Αιχμής

Ασφάλεια & Ανθρωπιά

Γνώση, Νόμος, Τάξη, Συντονισμός, Ισοτιμία, Αλληλεγγύη
Τμήματα Εξειδικευμένων Υπηρεσιών στην ΑΝΑΠΛΑΣΗ